Understanding Osteoporosis & Degenerative Kyphosis
Your bones are remarkable living tissues that support your entire body and its movements. Age and other conditions can cause your bones to lose mass and density—a condition called osteoporosis.
According to the National Osteoporosis Foundation, almost 54 million Americans either have osteoporosis or run the risk of developing it. More startling, this condition greatly increases your chance of sustaining broken bones. One in two women over the age of 50 with this disease will break a bone. Men are also at risk. In fact, about 25% of men with osteoporosis will suffer a bone fracture.
Osteoporosis can affect just about any bone in the body. The most common areas affected by this disease are the wrists, hips, knees, and spine. When the bones of the spine are weakened by osteoporosis, it can lead to a painful and disfiguring condition known as hyperkyphosis. This deformity occurs when the spinal bones compress or crack leading to a forward hunch in the thoracic spine.
So what exactly is osteoporosis and how can you prevent or treat this condition? Use our helpful guide to find out!
Understanding Osteoporosis
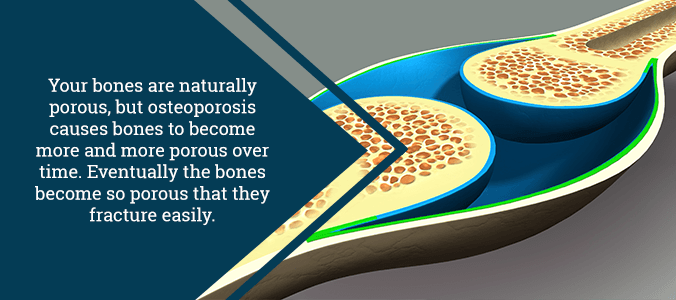
Some may view bones as solid structures that don’t change much after you reach adulthood. Bones are, in fact, made of living cells that are capable of growth and repair. The hard outer layer of each bone is called cortical bone. The spongy inner layer, known as trabecular bone, is less dense. When viewed with a microscope, a healthy bone resembles a honeycomb.
The term osteoporosis means “porous bones”. For those suffering from osteoporosis, the “honeycomb” has much larger holes and abnormal structures. This makes the bones weaker and more prone to fractures.
Types of Osteoporosis
Doctors typically divide osteoporosis into two different types based on the age of onset. These types include:
- Type 1 Osteoporosis: This type of osteoporosis generally affects women after the age of menopause. As estrogen levels decrease, the inner layer of trabecular bone begins to deteriorate. Women typically develop this condition after the age of 50. Bones in the wrist and spine are usually affected first.
- Type 2 Osteoporosis: Known as senile-onset osteoporosis, this type of the disorder affects adults over the age of 70. It involves the thinning of the inner and outer layers of cortical and trabecular bone. Women are twice as likely as men to develop this condition.
Causes & Risk Factors for Osteoporosis
As we age, our body’s production of hormones decreases. For women, the lack of estrogen after menopause is the main factor that contributes to osteoporosis. In addition, as men get older their testosterone levels sometimes decrease, leading to this disease.
However, hormones aren’t the only cause of osteoporosis. Knowing the lifestyle and health issues that hasten this disease is crucial to prevention. In fact, early screening for osteoporosis may be necessary if you have any of these risk factors:
- A family history of osteoporosis
- Inactive or sedentary lifestyle
- Diagnosis of kidney or liver disease
- Diagnosis of rheumatoid arthritis
- Eating disorders or poor nutrition
- Lack of calcium & vitamin D
- Digestive and gastrointestinal disorders where nutrients aren’t properly absorbed
- Issues with the thyroid, parathyroid, or adrenal glands
- Unhealthy habits like drinking and smoking
- Certain cancers like breast or prostate cancer
In addition, certain medications can cause osteoporosis. This includes the long-term use of certain blood thinners, oral corticosteroids, anti-seizure, or mood-enhancing drugs. If you feel you are at risk for osteoporosis, you should consult with your doctor. Knowing the risks and benefits of your medications will help you make more informed choices. This will also allow you to treat other conditions while minimizing your risk of osteoporosis.
Common Symptoms of Osteoporosis
Osteoporosis is considered a silent disease. Symptoms usually don’t occur until the disease has already caused significant damage to the bones. On occasion, people may experience tooth loss or receding gums if osteoporosis affects the jawbone. However, in cases of spinal osteoporosis, back pain due to a compression fracture is a common (and more obvious) symptom.
Some early warning signs that might indicate the onset of osteoporosis include weak and brittle fingernails or decreased hand grip strength. In addition, muscle and bone pain can be an indicator of a Vitamin D deficiency.
Loss of height is another common symptom of spinal osteoporosis. Likewise, developing a hunchback, known as kyphosis, can indicate issues with osteoporosis in the spine.
Osteoporosis & Degenerative Kyphosis
As osteoporosis thins spinal bones and weakens their structure, the vertebrae have a tendency to fracture. Typically, the front of the vertebra will collapse, losing its height, while the back remains relatively intact. These wedge-shaped vertebrae cause the spine to arc abnormally forward. This abnormal spinal curvature from osteoporosis is known as a degenerative kyphotic spine.
Mild kyphosis may only result in some stiffness or back pain. As the spinal bones continue to weaken, however, this abnormal curvature of the spine only worsens. It could lead to more serious pain as well as breathing problems due to pressure on the lungs. In addition, as the front of the bone continues to be crushed, the back muscles weaken. This makes it difficult to perform normal tasks like walking or standing up. The unnatural curvature of the spine may also make driving and lying down more difficult.

Preventing Osteoporosis
Fortunately, there are some things that you can do to prevent osteoporosis. Be aware of your family history as well as the risk factors mentioned above.
If you have one or more risk factors or are advancing in age, it is advisable to get a bone mineral density test. This test uses x-rays to measure the minerals present in your bones. It is a simple test where you lie on a table as special x-rays are taken. Preventive screening of a mineral bone density test is recommended for all women over the age of 65. Those at risk for osteoporosis may require this test even sooner.
In addition to routine screenings, adopting a healthy lifestyle can increase bone density. This includes quitting smoking and limiting your daily alcohol intake. Studies have shown that exercise is very effective in increasing bone density. Weight-bearing and aerobic exercises like walking, climbing stairs, or jogging are great options. If you have more severe osteoporosis, then you will want to consult with a doctor or other specialists before embarking on an exercise program. This discussion will prevent injury or any further damage from occurring to the bones.
In addition, a healthy diet with the proper calcium and vitamin D helps keep the bones strong. Calcium is found in milk, yogurt, dark green vegetables, grains, and beans. Vitamin D comes from exposure to sunlight, fatty fish, and fortified foods like cereals, milk, and orange juice. Talk to your doctor about using calcium and vitamin D supplements.
Treatment Options for Osteoporosis & Degenerative Kyphosis
After receiving a thorough physical exam including a complete medical history and diagnostic imaging, your doctor will then determine your most appropriate treatment options. These options may include education on the condition and lifestyle changes to prevent bone fractures.
Several medications have proven effective in treating osteoporosis. According to the International Osteoporosis Foundation, medications can reduce your risk of sustaining an osteoporotic fracture by 30-70%. In fact, USDA approved medications may even slow down or stop bone loss entirely as well as increase bone formation. Consult with your doctor to determine which medication is best for your specific condition.
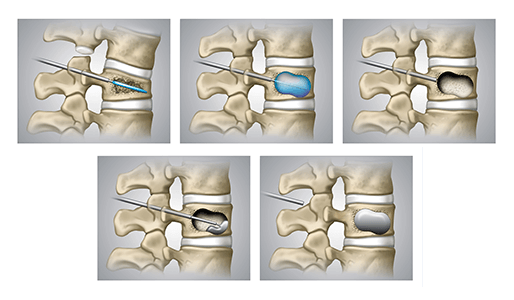
In more severe cases, surgical procedures can help to stabilize fractured or broken vertebrae. Vertebroplasty uses specialized bone cement to harden the fractures and support the spine. Likewise, another even newer treatment, kyphoplasty, uses special balloons to expand the compressed bone. Then, your doctor will inject cement into the expanded areas.
These minimally invasive procedures help to relieve pain, restore height, and reduce spinal deformity.
Finding Treatment for Your Degenerative Kyphosis & Osteoporosis
If osteoporosis has left you with painful spinal issues, then you’ll want to find the best treatments to help you get your life back. Dr. Jason Lowenstein is a leading expert in minimally invasive spinal deformity care, including degenerative kyphosis treatment. Voted a Top Doctor by New Jersey Monthly Magazine and Inside Jersey Magazine, Dr. Lowenstein delivers compassionate, patient-centered care for a variety of spinal deformities.
Get the help you need by scheduling an appointment today!
