Treating Scoliosis in Children with Cerebral Palsy (CP)
Scoliosis is a spine disorder that is known to cause unusual changes in the curvature of the spine. If left untreated, the spine becomes more deformed, leading to severe health problems later in life. Children who suffer from cerebral palsy (CP) have a much higher incidence of developing moderate to severe scoliosis during their early years. This is because balance issues and muscle weakness are common in children with CP. In children with CP, scoliosis will continue to progress along with skeletal maturity. This is in contrast to idiopathic scoliosis, which does not progress much after skeletal growth.
Conservative treatments may slow down curve progression, although scoliosis surgery is usually recommended for definitive management. Surgical techniques have advanced over the last several decades to allow for more effective treatment. Additionally, complications rates have decreased greatly, although this always depends on the case at hand.
Characteristics of Cerebral Palsy (CP)
CP is a disorder that affects movement, posture, or muscle tone and is caused by damage that occurs to the developing brain. Most commonly, this damage occurs before birth. Signs and symptoms may appear during infancy or when the child is in preschool. CP’s effect on functionality varies extensively. Some people with CP can walk while others cannot. Additionally, some may show normal intellectual development, while others have intellectual disabilities.

Symptoms of Cerebral Palsy (CP)
Signs and symptoms of CP vary greatly between cases. Movement and coordination problems may include:
- Variations in muscle tone
- Spasticity (stiff muscles and exaggerated reflexes)
- Rigidity (stiff muscles with normal reflexes)
- Ataxia (Lack of muscle coordination)
- Athetosis (Slow, writhing movements)
- Seizures
- Tremors or involuntary movements
- Difficulty walking
- Favoring one side of the body
- Paraplegia
- Difficulty speaking, eating, or swallowing
- Difficulty with fine motor muscle control
CP may affect one limb or one side of the body. Additionally, it may affect the body as a whole. Thankfully, CP doesn’t change with time, so the symptoms usually do not worsen with age. That being said, muscle rigidity and shortening may worsen with time if left untreated.
Causes of Cerebral Palsy (CP)
CP occurs during brain development, usually before the child is born. Most of the time, the exact trigger is unknown. That being said, there are contributing factors that may lead to brain development problems such as:
- Maternal infections that affect fetal development
- Mutation in genes leading to abnormal brain development
- A disruption of blood supply to the developing brain due to fetal stroke
- Traumatic head injury to the infant from a fall or other accident
- Birth-related asphyxia

Characteristics of Scoliosis
Scoliosis is a sideways curvature of the spine that is known to occur most commonly during the growth spurt before puberty. Most cases are categorized as mild scoliosis, but the condition can worsen as a child grows. Additionally, severe forms of the condition can lead to disability. In extreme cases, spinal curvature can reduce the amount of space within the chest, making it difficult to breathe. Likewise, both CP and neuromuscular disorders in general may lead to scoliosis, however, the cause of most scoliosis cases is unknown.
For the sake of relevance, this section will focus on neuromuscular scoliosis (NSC). This form of the condition is relevant as it is caused by disorders of the spinal cord, brain, and muscular system (such as CP). With neuromuscular scoliosis, muscles and nerves cannot maintain proper balance or alignment of the spine and trunk. The condition often occurs with pelvic obliquity, where the child’s pelvis becomes unevenly tilted. Additionally, kyphosis often exists concurrently with NSC.
Symptoms of Neuromuscular Scoliosis (NSC)
Not all children with neuromuscular conditions develop NSC. That being said, it is not entirely uncommon either. In children with CP, there is a 25% chance that NSC will develop concurrently. The chance of developing NSC is greater in patients who require the use of wheelchairs. With some neuromuscular conditions, a child may need wheelchair assistance upon reaching adolescence. It is at this time when the child is at the most risk for developing NSC or curve progression. Naturally, this is because this time is often associated with major growth spurts.
For children who are able to walk, NSC has similar symptoms to those with idiopathic scoliosis:
- Rib prominence on one side of the body
- Uneven waistline
- One hip is noticeably higher than the other
- Uneven shoulders, usually with one shoulder blade protruding more than the other
Children in wheelchairs (the ones at the greatest risk) may have any number of the symptoms above, as well as:
- Pelvic obliquity (tilted pelvis)
- Development of pressure sores due to overall imbalance and pelvic tilt
- Change in overall posture (leaning or slouching more to one side)
- Hindered ability to sit (may need to use arms and hands for seating support)
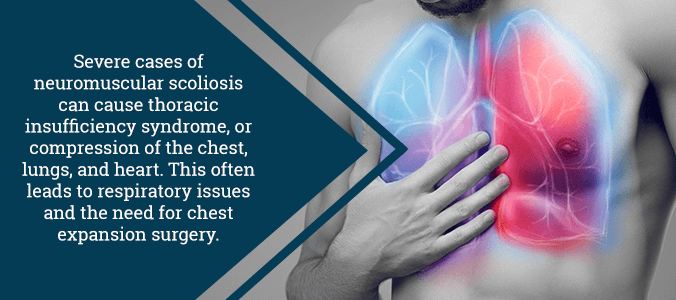
These changes can affect a child’s independence, making daily activities such as dressing and eating more difficult. Additionally, children with NSC may have other spinal deformities, such as thoracic kyphosis or lumbar lordosis. Larger scoliotic curves in the upper back may reduce space in the chest, which can cause respiratory problems.
Additionally, curve magnitude divides into 3 groups:
- Group-I Curves: Curves smaller than 25 degrees
- Group-II Curves: Curves between 25 and 35 degrees
- Group-III Curves: Curves greater than 35 degrees
Nonsurgical Treatments for Scoliosis with CP
Although these treatments do not prevent curve progression, they may delay progression and improve quality of life. Nonsurgical treatments include:
- Back Braces for Scoliosis: For patients in wheelchairs, a doctor may recommend a molded plastic brace worn around the upper body. This brace will allow for more stability while sitting down. Additionally, the brace also allows for more comfortable use of the extremities while reclining. That said, bracing does not prevent curve progression in NSC as it does with idiopathic scoliosis.
- Wheelchair Modification: This is a very commonly recommended form of nonsurgical treatment. If your child’s balance is affected by an uneven pelvis, his or her wheelchair can be customized to promote better posture. Modifications such as this may include individualized chair molds and additional adjustment tools. The latter, in this case, is normally implemented to help improve balance while sitting.
- Physical Therapy: Specific exercises may help a patient with muscular imbalances and it can improve motor functioning.
NSC patients who are able to walk may find that braces negatively affect their sense of balance or walking stability. This is especially true if they have muscle weakness, an unsteady gait, or pulmonary complications.

Surgical Treatments for Scoliosis with CP
Your doctor will usually only consider surgery after more conservative options have been exhausted. The team of specialists treating your child will determine whether to recommend surgery or not. They will consider things such as the severity of the condition and its impact on your child’s daily functioning. The most common prerequisites for surgery are:
- Pain
- Difficulty sitting and loss of function
- Problems with the lung or heart
- Curves greater than 50 degrees in growing patients
- Curve progression of more than 10 degrees in patients with 50 degree curves
The decision to proceed with surgery in noncommunicative patients is often very difficult. In such cases, the decision to perform a procedure relies on the size on the spinal curve, the care of the patient, and the impact of the curve on sitting balance. The goals of surgical stabilization are:
- Reduce pain
- Improve breathing
- Stabilize the curve and stop curve progression
- Balance the spine and the pelvis
Patients can usually achieve these goals using the following methods:
Growing Rods
A doctor may use growing rods to temporarily stabilize the spine. Additionally, growing rods relieve pressure in the chest, lungs, and spine by allowing them more space to grow The goal of a growing rod is to promote growth while simultaneously correcting the curve.
During this procedure, one or two rods are attached at the top and bottom of the curve. Every 6 to 8 months the child returns to the doctor for a minor rod-lengthening procedure. This is to keep up with growth. When the child finishes growing, the rods are removed and a spinal fusion procedure is performed.
Spinal Fusion
Spinal fusion surgeryis the most widely used surgical treatment for NSC. During the surgery, your doctor will connect the abnormal vertebrae together so that they heal into a single bone. This stops growth completely in the affected segment of the spine and it prevents worsening of the curve. Next, the performing doctor places tiny bits of bone graft between the vertebrae to allow for fusion. These grafts are obtained from a bone bank or are made using artificial materials. Over time, the bone grows into a single, solid strip.
Metal rods are often used in place until the bones connect. The rods bind to the spine through the use of hooks, screws, and/or wires. Once the bone graft fuses together, the spine stabilizes and the condition no longer progresses.
Lastly, because patients in wheelchairs generally have a pelvic tilt, fusion may be needed in other parts of the body. For example, multi-level spinal fusion may extend from the upper thoracic spine down to the pelvis.
Does your child have NSC? If so, please call (855) 220-5966 or make an appointment online. Dr. Jason E. Lowenstein is a board-certified, fellowship-trained scoliosis surgeon with over a decade of expertise.
